

We are a premium London provider of melasma treatment in London, so get in touch to find out how we can help you.
Melasma (also known as chloasma) is a kind of hyperpigmentation disorder. It’s characterised by tan or brown patches occurring most commonly on the face.
The hyperpigmentation typically forms in a symmetrical pattern in sun-exposed areas such as on the forehead, nose, cheeks, chin and upper lip.
Melasma is more common in women than men, and in people with darker skin types. Thankfully, it is a harmless condition and not painful.

At the cellular level, disorders of pigmentation are caused by excess melanin (the skin pigment), which then spreads outside the normal containment mechanisms in the skin structure.
These conditions do not pose a serious medical threat, but they can have psychological impacts and understandably be upsetting.
While it may not be possible to cure melasma permanently, effective melasma treatment is available to help manage the condition.
Hormonal fluctuations are among the key melasma causes, as seen by the link with pregnancy. The contraceptive pill, hormone therapies, menopause, other conditions that affect the hormones (such as thyroid problems) are all triggers. Some medications (e.g. treatments for epilepsy) and even using the wrong cosmetics, have also been associated with the condition.
Exposure to the sun can trigger melasma or make a pre-existing condition worse. As a general rule, patients experience flare-ups in the summer months, rather than in winter. Those who tan well, or with darker skin tones, are more likely to experience melasma.
There is also evidence to suggest that family history may be a risk factor, with some studies finding that over half of patients with melasma have a positive family history.
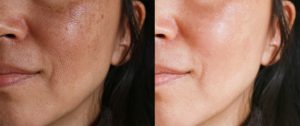
Melasma on the face is particularly common in pregnant women. According to the British Association of Dermatologists, up to 50% of pregnant women may be affected. For this reason, it has acquired its own informal description for this context: ‘the pregnancy mask’.
There is no substitute for an experienced eye when it comes to diagnosing melasma. In the case of dark patches on the face, as opposed to other areas of the body, a symmetrical pattern on either side may provide a helpful clue.
A dermatologist is the best port of call for a definitive diagnosis and melasma treatment.
Aside from identifying the condition by visual examination, the dermatologist may conduct an examination using a hand-held microscope known as a dermascope, with imaging capabilities.
More sophisticated diagnostic techniques that may be deployed include digital imaging platforms. These can provide an instant, painless and accurate view beneath the surface of the skin, without the need for a surgical biopsy.
Melasma treatment can be challenging, and what works for one patient may not work for another.
However while a cure may not always be possible, the condition can certainly be effectively managed. Often, the best treatment for melasma is a combination of approaches that will improve the appearance of affected skin.
A sure-fire recommendation, in every case, is to limit sun exposure. Melasma cannot be treated or prevented without the help of good sun protection habits. Most dermatologists will advise regular application of sunscreen (SPF30 or higher) and wearing a hat when exposed to the sun.
Topical treatments, such as hydroquinone, corticosteroids and azelaic acid may be effective, and oral medications might also be prescribed. Other treatments, such as phototherapy (light and laser treatment) can also be applied to excellent effect, under the supervision of an experienced dermatologist.
In most cases, pregnancy-related melasma often disappears soon after giving birth. However, in some cases – especially where there is sun exposure – it may take many months to fade away. Skin type and hormone levels may also play a part in changes to the epidermis.
Our Clinic’s founder Dr Haus, has many years experience of managing melasma and other hyperpigmentation conditions. Trained in Brazil, where there are many different tones and types of skin, as well as lots of sun, he has what might be considered the ideal professional pedigree to treat melasma.
We offer many of the most popular treatments for pigmentation, and have also pioneered revolutionary gold standard treatments that target pigment producing cells.
Dr Haus Dermatology in Harley Street was the first clinic in the UK to offer patients ‘elos’ laser treatment technology. This state-of-the-art platform delivers laser, light and radio frequencies to treat melasma and other hyperpigmentation conditions.
Other melasma laser treatments include the Erbium and Fraxel laser modalities. the new SmartPICO, laser Chemical peels, microneedling and drug delivery, are other effective tools in the Dr Haus Dermatology treatment kit.
If you are struggling with skin discolouration symptoms that may indicate melasma, contact us at Dr Haus Dermatology for more information about our services.
Our experience with this frequently distressing condition means we understand your concern, and can help you to decide the right next step for you.